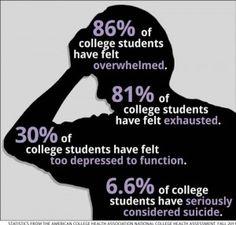
 Although mental health counseling centers and awareness services exist on many campuses, if students and staff do not know about these services, do not have the tools to help themselves, and do not have the tools to help someone else in distress, these resources go unused. Hunt and Eisenberg (2010) indicate that while many college students are seen as being more privileged than their non-student peers, there is very little difference in the occurrence of mental health problems between the two groups. According to the authors, college attendance in high school graduates is at 65%. Among people age 18-24, half of all health concerns are related to mental illness. Also, onset generally occurs by the age of 24. This is a prime time for college administrators to recognize and intervene with mental health issues. Untreated mental health affects academic success, productivity, substance abuse, and relationships. Because students are often immersed in campus life including their involvement in academics, recreational activities, social interactions, and work, they are well known by their peers and by staff, who can serve as allies when needed (Wagner and Rhee, 2013).
Although mental health counseling centers and awareness services exist on many campuses, if students and staff do not know about these services, do not have the tools to help themselves, and do not have the tools to help someone else in distress, these resources go unused. Hunt and Eisenberg (2010) indicate that while many college students are seen as being more privileged than their non-student peers, there is very little difference in the occurrence of mental health problems between the two groups. According to the authors, college attendance in high school graduates is at 65%. Among people age 18-24, half of all health concerns are related to mental illness. Also, onset generally occurs by the age of 24. This is a prime time for college administrators to recognize and intervene with mental health issues. Untreated mental health affects academic success, productivity, substance abuse, and relationships. Because students are often immersed in campus life including their involvement in academics, recreational activities, social interactions, and work, they are well known by their peers and by staff, who can serve as allies when needed (Wagner and Rhee, 2013).
Hunt and Eisenberg (2010) report that one in three college students have reported that they have experienced depression symptoms that have resulted in a significant life impact. Of those students, 4% admitted to having seriously considered suicide. Anxiety is another common challenge on college campuses. Academics are becoming more competitive as the prospects for employment following college are decreasing. Stress is increasing as a result. While the effects of stress are often minor and common among college students (go here for further reading), there is nevertheless a lurking danger, and in severe cases, treatment is necessary. Many students are dealing with critical levels of stress on college campuses, and this is a concerning reality.
Many campus administrators and counselors are of the opinion that they are providing appropriate information on mental health to promote awareness and prevention. However, the study by Wagner and Rhee (2013) does not bear this out. Students are likely to report that they do not find the information helpful in self-identification or in recognizing problems in others. This is a mistake given the close relationships that tend to occur on campuses. Students are interested in information on depression and anxiety, grief, stress, sleep, and relationship difficulties in addition to information on how to help others. This is a fertile population to educate as they spend considerable education and social time together.
In a study on school based mental health which is more focused on primary education, there are trends that translate to similar issues at the college level (Weist, 2005). The findings of this study indicate that mental health services were not a focus and were not well funded. Assessment of needs and linking to services are not done effectively. Educators can certainly be promoters of mental health awareness but time and resources are limited. At the college level, these effects may be amplified. However there is great opportunity to catch mental health concerns early and before they become more severe.
Dogan (2012) points out that many mental health problems emerge in the first year of college because it is a difficult time of transition in the lifespan. There is more freedom, different types of support systems, and increased stress. College students are often struggling to find a good balance between education and social interactions. The authors also found that students are increasingly presenting with more intense problems, and that as time goes on toward graduation, stress levels and mental health issues increase dramatically. Self-referral continues to be the main avenue to first contact, but that parents, staff, and friends are also making referrals.
Given all of the above, there has been a focus on campaigns to increase awareness and to decrease the stigma of diagnosis and treatment (Livingston, et al., 2012). This was shown to make individuals more aware of problems, but did not necessarily decrease stigma which can lower the likelihood that an individual will seek treatment. Perhaps it is important for universities to change the way that they approach promotion of mental health awareness. Asking students and staff what they need for themselves and in order to help others seems to be a significant step. While this may work now, it may need to be fluid and change over the years. It also makes sense for information to be disseminated in such a way that all staff and students know where to turn if experiencing a mental health problem, or when they recognize a problem in another individual. Finally, universities can hope to succeed in the promotion of mental health if they provide the staff the necessary training and resources for that success.
By Christie Hunter
Souces:
Dogan, T. (2012). A long-term study of the counseling needs of Turkish university students. Journal of Counseling and Development : JCD, 90(1), 91-96.
Hunt, J., Eisenburg, D. (2010). Mental health problems and help-seeking behavior among college students. Journal of Adolescent Health, 46(1), 3-10.
Livingston, J. D., Tugwell, A., Korf-uzan, K., Cianfrone, M., & Coniglio, C. (2013). Evaluation of a campaign to improve awareness and attitudes of young people towards mental health issues. Social Psychiatry and Psychiatric Epidemiology,48(6), 965-73.
Wagner, M., & Rhee (2013). Stress, sleep, grief: Are college students receiving information that interests them? College Student Journal, 47(1), 24-33.
Weist, M. D. (2005). Fulfilling the promise of school-based mental health: Moving toward a public mental health promotion approach. Journal of Abnormal Child Psychology, 33(6), 735-41.


 This past Tuesday, the Women's Health Research Institute welcomed U.S. Rep. Jan Schakowsky in the celebration of the recently announced National Institutes of Health (NIH) and Food and Drug Administration policies to include women in basic science and clinical studies. The event attracted over 200 guests and WHRI Director Teresa Woodruff, PhD shared the floor with Congresswoman Schakowsky and Jay Walsh, PhD, Vice President for Research at Northwestern University.
This past Tuesday, the Women's Health Research Institute welcomed U.S. Rep. Jan Schakowsky in the celebration of the recently announced National Institutes of Health (NIH) and Food and Drug Administration policies to include women in basic science and clinical studies. The event attracted over 200 guests and WHRI Director Teresa Woodruff, PhD shared the floor with Congresswoman Schakowsky and Jay Walsh, PhD, Vice President for Research at Northwestern University. 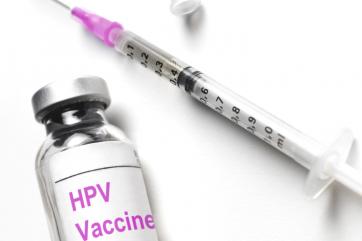 Protect your daughter from cervical cancer by getting her the HPV vaccine. It takes 3 shots to complete the series, so make sure she gets them all to be protected. It's easy to get very busy with school, activities, work, and all of the juggling that parents of preteens and teens do every day. However, for the sake of your daughter's health, it's important to take the time to get her the life-saving HPV vaccine to protect against cervical cancer. Every year in the United States about 12,000 women are diagnosed with cervical cancer, and 4,000 die. If we protect girls now, we could reduce disease and cancer due to HPV.
Protect your daughter from cervical cancer by getting her the HPV vaccine. It takes 3 shots to complete the series, so make sure she gets them all to be protected. It's easy to get very busy with school, activities, work, and all of the juggling that parents of preteens and teens do every day. However, for the sake of your daughter's health, it's important to take the time to get her the life-saving HPV vaccine to protect against cervical cancer. Every year in the United States about 12,000 women are diagnosed with cervical cancer, and 4,000 die. If we protect girls now, we could reduce disease and cancer due to HPV. Over the past several years, gluten free diets have been all the rage. Is it true that gluten free diets can help you lose weight or is this just a fad? Gluten is a protein present in foods including wheat, rye, oats, and barley, but may also be found in everyday products such as medicines, vitamins, and even lip balms. There's absolutely nothing wrong with eating gluten unless you have celiac disease, or gluten sensitive enteropathy (GSE), an autoimmune disease that damages the small intestine and interferes with absorption of nutrients from food. If you are sensitive to gluten, the body produces an abnormal immune response to it, attacking the lining of small intestine where digestion takes place. This leads to the symptoms of celiac disease:
Over the past several years, gluten free diets have been all the rage. Is it true that gluten free diets can help you lose weight or is this just a fad? Gluten is a protein present in foods including wheat, rye, oats, and barley, but may also be found in everyday products such as medicines, vitamins, and even lip balms. There's absolutely nothing wrong with eating gluten unless you have celiac disease, or gluten sensitive enteropathy (GSE), an autoimmune disease that damages the small intestine and interferes with absorption of nutrients from food. If you are sensitive to gluten, the body produces an abnormal immune response to it, attacking the lining of small intestine where digestion takes place. This leads to the symptoms of celiac disease: Although mental health counseling centers and awareness services exist on many campuses, if students and staff do not know about these services, do not have the tools to help themselves, and do not have the tools to help someone else in distress, these resources go unused. Hunt and Eisenberg (2010) indicate that while many college students are seen as being more privileged than their non-student peers, there is very little difference in the occurrence of mental health problems between the two groups. According to the authors, college attendance in high school graduates is at 65%. Among people age 18-24, half of all health concerns are related to mental illness. Also, onset generally occurs by the age of 24. This is a prime time for college administrators to recognize and intervene with mental health issues. Untreated mental health affects academic success, productivity, substance abuse, and relationships. Because students are often immersed in campus life including their involvement in academics, recreational activities, social interactions, and work, they are well known by their peers and by staff, who can serve as allies when needed (Wagner and Rhee, 2013).
Although mental health counseling centers and awareness services exist on many campuses, if students and staff do not know about these services, do not have the tools to help themselves, and do not have the tools to help someone else in distress, these resources go unused. Hunt and Eisenberg (2010) indicate that while many college students are seen as being more privileged than their non-student peers, there is very little difference in the occurrence of mental health problems between the two groups. According to the authors, college attendance in high school graduates is at 65%. Among people age 18-24, half of all health concerns are related to mental illness. Also, onset generally occurs by the age of 24. This is a prime time for college administrators to recognize and intervene with mental health issues. Untreated mental health affects academic success, productivity, substance abuse, and relationships. Because students are often immersed in campus life including their involvement in academics, recreational activities, social interactions, and work, they are well known by their peers and by staff, who can serve as allies when needed (Wagner and Rhee, 2013). Dental health is often overlooked or thought of once a year in our annual cleaning in the dentist’s office. But practicing good oral care can save you expensive dental repair procedures down the road! Three simple steps can help you keep your mouth healthy. First things first, saliva is the most important barrier against germs. Saliva is rich in antibacterial properties that kill germs and heal wounds. Keeping your mouth healthy means keeping your saliva levels healthy. If you suffer from dry mouth, you may be opening the door wide for gum-disease! Some medications may cause dry-mouth, so combat these with sugar free gum to help get the saliva flowing. Regularly rinsing out your mouth with water will help wash away any lingering food particles that attract bacteria. Bacteria can cause plaque, cavities, gingivitis, and gum disease. Swishing water around your mouth after and between meals can actually make a big difference in dental health! Stress is an unexpected culprit of dental problems, but nevertheless is linked to almost all types of oral problems. Chronic tension and stress weakens the body’s immune system, which makes fighting infections (including oral infections) more difficult. Stress also can trigger increased acid levels in your mouth, which makes cavities more likely. Take a moment to change the way you think about oral hygiene, and show those pearly whites proudly! Source:
Dental health is often overlooked or thought of once a year in our annual cleaning in the dentist’s office. But practicing good oral care can save you expensive dental repair procedures down the road! Three simple steps can help you keep your mouth healthy. First things first, saliva is the most important barrier against germs. Saliva is rich in antibacterial properties that kill germs and heal wounds. Keeping your mouth healthy means keeping your saliva levels healthy. If you suffer from dry mouth, you may be opening the door wide for gum-disease! Some medications may cause dry-mouth, so combat these with sugar free gum to help get the saliva flowing. Regularly rinsing out your mouth with water will help wash away any lingering food particles that attract bacteria. Bacteria can cause plaque, cavities, gingivitis, and gum disease. Swishing water around your mouth after and between meals can actually make a big difference in dental health! Stress is an unexpected culprit of dental problems, but nevertheless is linked to almost all types of oral problems. Chronic tension and stress weakens the body’s immune system, which makes fighting infections (including oral infections) more difficult. Stress also can trigger increased acid levels in your mouth, which makes cavities more likely. Take a moment to change the way you think about oral hygiene, and show those pearly whites proudly! Source: 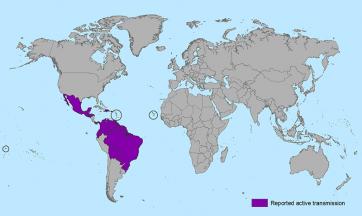 The Zika virus has had a lot of press recently, and it is important to understand the facts surrounding this virus. The Zika virus is transmitted by mosquitoes and can cause a fever, rash, joint pain, or head ache. Most troublingly, this virus is suspected to lead to birth defects if a pregnant mother contracts Zika. While there is currently no vaccine to prevent Zika, you can best protect yourself by avoiding mosquito bites when traveling to countries where this virus is found. Zika has primarily spread in South America and Central America, with a few exceptions.
The Zika virus has had a lot of press recently, and it is important to understand the facts surrounding this virus. The Zika virus is transmitted by mosquitoes and can cause a fever, rash, joint pain, or head ache. Most troublingly, this virus is suspected to lead to birth defects if a pregnant mother contracts Zika. While there is currently no vaccine to prevent Zika, you can best protect yourself by avoiding mosquito bites when traveling to countries where this virus is found. Zika has primarily spread in South America and Central America, with a few exceptions.