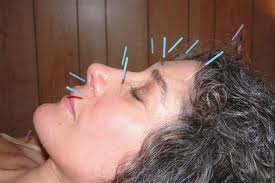
 Acupuncture provides more relief from various types of chronic pain than does usual care and should be considered a valid therapeutic option, according to Andrew J. Vickers, DPhil of Memorial Sloan Kettering in NYC and colleagues who conducted a meta-analysis of raw data from 29 studies.
Acupuncture provides more relief from various types of chronic pain than does usual care and should be considered a valid therapeutic option, according to Andrew J. Vickers, DPhil of Memorial Sloan Kettering in NYC and colleagues who conducted a meta-analysis of raw data from 29 studies.
For back and neck pain, osteoarthritis, and chronic headache, pain scores among patients treated with acupuncture were below the pain scores for patients receiving sham acupuncture. The pain score improvement was even larger when acupuncture was compared with no acupuncture, the researchers reported online in Archives of Internal Medicine.
Acupuncture is recognized as having certain physiologic effects that can contribute to pain relief, but no plausible mechanism has been identified that could lead to long-term benefits for chronic pain, with the result that the treatment remains "highly controversial," according to the researchers. Many controlled studies of acupuncture for pain have been published, but quality has been inconsistent and reliability has been questioned.
To provide more clarity about the effects of acupuncture on pain, Vickers and colleagues conducted an individual patient data meta-analysis based exclusively on high quality randomized trials. Included trials required pain of at least a month's duration, with the primary endpoint being assessed at least a month after acupuncture treatment began.
This is "of major importance for clinical practice," meaning that acupuncture should be considered "a reasonable referral option for patients with chronic pain," they stated.
In an invited commentary accompanying the meta-analysis, Andrew L. Avins, MD, of Kaiser-Permanente in Oakland, Calif., argued that the benefits indeed were primarily those associated with the placebo effect, because the pain relief was so much greater when acupuncture was compared with usual care than when compared with the sham procedure.
But whether that should mean acupuncture has no value for patients, largely because of uncertainty as to its mechanisms of action, is a crucial concern, he pointed out.
"The ultimate question is: does this intervention work (or, more completely, do its benefits outweigh its risks and justify its cost)?" Avins wrote.
For acupuncture, the current meta-analysis offers "some robust evidence" that acupuncture does provide greater chronic pain relief than usual care, mechanisms of effect aside.
"Perhaps a more productive strategy at this point would be to provide whatever benefits we can for our patients, while we continue to explore more carefully all mechanisms of healing," Avins concluded.
Primary source: Archives of Internal Medicine
Vickers A, et al "Acupuncture for chronic pain: individual patient data meta-analysis" Arch Intern Med 2012; DOI: 10.1001/archinternmed.2012.3654.
Additional source: Archives of Internal Medicine
Avins A "Needling the status quo" Arch Intern Med 2012; DOI: 10.1001/archinternmed.2012.4198.

 Being physically active is one of best ways people with arthritis can improve their health, but a new study from Northwestern University Feinberg School of Medicine shows that more than half of women and 40 percent of men with arthritis are virtually couch potatoes.
Being physically active is one of best ways people with arthritis can improve their health, but a new study from Northwestern University Feinberg School of Medicine shows that more than half of women and 40 percent of men with arthritis are virtually couch potatoes.
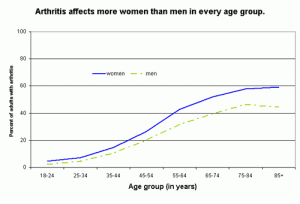 In 2006, the Center for Disease Control and Prevention (CDC) reported that 21.6% of the US adult population reported arthritis, with significantly higher prevalence in women than in men (24.4% vs. 18.1%). Arthritis prevalence increased with age and was higher among women than men in every age group. With the aging of the US population, the prevalence of doctor-diagnosed arthritis is expected to increase in the coming decades. By 2030, it is estimated that 67 million adults age 18 and older will have arthritis, compared with the current 46 million. Also, by 2030 an estimated 25 million adults will report arthritis-attributable activity limitations.
In 2006, the Center for Disease Control and Prevention (CDC) reported that 21.6% of the US adult population reported arthritis, with significantly higher prevalence in women than in men (24.4% vs. 18.1%). Arthritis prevalence increased with age and was higher among women than men in every age group. With the aging of the US population, the prevalence of doctor-diagnosed arthritis is expected to increase in the coming decades. By 2030, it is estimated that 67 million adults age 18 and older will have arthritis, compared with the current 46 million. Also, by 2030 an estimated 25 million adults will report arthritis-attributable activity limitations.