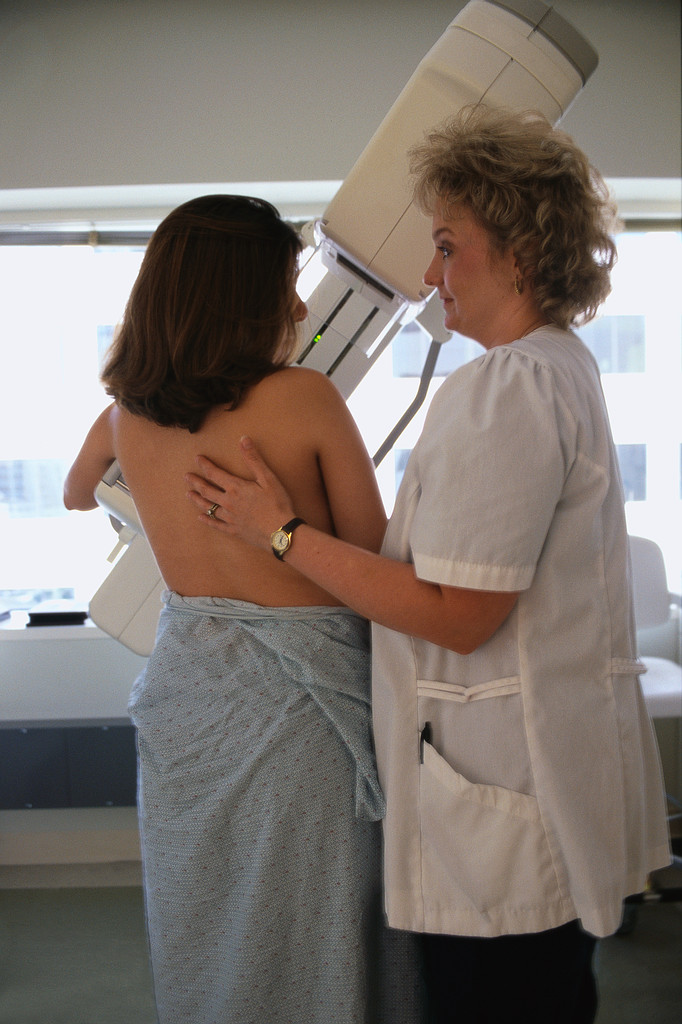
You may have noticed the NFL players wearing their pink gloves and shoes for Breast Cancer Awareness Month. But did you know that breast cancer is the leading cause of cancer-related deaths in American women? It is caused by abnormal cell growth in the breast tissue, usually beginning in the milk-producing ducts. The abnormal growth may spread (metastasize) through your breast to your lymph nodes, or other parts of your body.
 The most common symptom of breast cancer in both men and women is a lump in the breast, which is usually painless. Most breast lumps are non-cancerous, but it is still important to have any lumps evaluated by a physician. Other symptoms of breast cancer include clear or bloody discharge from the nipple, change in breast size or shape, retraction or indentation of the nipple and skin around the breast. Treatment for breast cancer often involves surgery, radiation therapy, and/or chemotherapy. A variety of surgical techniques are available depending on the size of the lump or tumor.
The most common symptom of breast cancer in both men and women is a lump in the breast, which is usually painless. Most breast lumps are non-cancerous, but it is still important to have any lumps evaluated by a physician. Other symptoms of breast cancer include clear or bloody discharge from the nipple, change in breast size or shape, retraction or indentation of the nipple and skin around the breast. Treatment for breast cancer often involves surgery, radiation therapy, and/or chemotherapy. A variety of surgical techniques are available depending on the size of the lump or tumor.
The good news is there are many resources for breast cancer treatment and research at Northwestern!
The Lynn Sage Cancer Research Foundation in partnership with Northwestern Memorial Hospital and the Robert H Lurie Comprehensive Cancer Center has established the Lynn Sage Breast Cancer Program to provide women with access to the latest advances and technology in breast cancer treatment. The center offers clinical, diagnostic, rehabilitation and counseling services at a single location.
Northwestern Memorial Hospital also offers breast reconstruction surgery for patients who have undergone lumpectomy or mastectomy or who have other cancer-related deformities. Dr. Neil Fine, a plastic surgeon at NMH has developed an innovative technique as an alternative to total mastectomy. The technique involves repositioning portions of the latissimus dorsi into the breast where a tumor has been removed. Only a handful of other hospitals across the country are offering this procedure.
http://www.nmh.org/nmh/home.htm
IWHR Highlighted Researcher
Dr. Seema A. Khan M.D., is the Bluhm Family Professor of Cancer Research at Northwestern University’s Feinberg School of Medicine. She is also the Director of the Bluhm Family Breast Cancer Early Detection and Prevention Program at Feinberg. She received her medical degree from Dow Medical College in Pakistan and a Master’s in Epidemiology from the Harvard School of Public Health. Dr. Khan is a board-certified surgeon whose research interests involve prevention, early detection and treatment of breast cancer. Currently she has multiple active clinical trials including a study designed to identify biomarkers for breast cancer risk in benign breast tissue. Similarly, she is investigating the level of estrogen in nipple fluid as a marker for breast cancer risk. Other recent studies include the development of a topical treatment for non-invasive breast cancer and the multi-center evaluation of a preventive breast cancer therapy for post-menopausal women taking Hormone Replacement Therapy.
Other Useful Links and Resources:
http://www.breastcancer.org/
http://www.cancer.gov/cancertopics/types/breast
http://www.nlm.nih.gov/medlineplus/breastcancer.html
http://www.komen.org/