 Currently, 60% of women are using birth control (with over 99% of women having used it in their lifetime)--from the pill, hormone shots, and non-hormonal methods (like the diaphragm). But now, more and more women are turning to intrauterine devices (IUDs) as their choice of contraception. The Centers for Disease Control and Prevention recently released a survey that showed between 2002-2013, the number of women using the pill, condoms, and female sterilization has dropped and the number of women using long-acting contraceptives (IUDs or contraceptive implants) has more than quadrupled!
Currently, 60% of women are using birth control (with over 99% of women having used it in their lifetime)--from the pill, hormone shots, and non-hormonal methods (like the diaphragm). But now, more and more women are turning to intrauterine devices (IUDs) as their choice of contraception. The Centers for Disease Control and Prevention recently released a survey that showed between 2002-2013, the number of women using the pill, condoms, and female sterilization has dropped and the number of women using long-acting contraceptives (IUDs or contraceptive implants) has more than quadrupled!
Once inserted, IUDs can be reliable for years without having to be replaced or tampered with. The convenience with IUDs is that there is little or no room for human error--no pill to remember, no contraception device to travel with--it just stays in your body to prevent pregnancy. The rise of IUD use is a little surprising, given that women in the United States have been slower to accept implants than women in other countries. This hesitancy was due in large part to misconceptions regarding IUDs being difficult to implant and causing infections. Despite these misconceptions (which have been around for over 30 years), women are starting to trust IUDs as the most effective form of birth control. It's important to remember that while IUDs are effective in reducing the risk of pregnancies, IUDs do not protect against sexually transmitted infections.
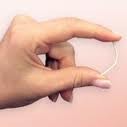
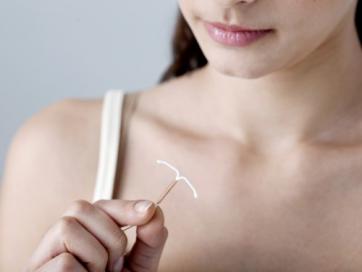
An IUD is a T-shaped device implanted into the uterus for the purpose of contraception by preventing sperm from reaching the egg. There are four different IUDs available in the United States. Three of them, Liletta, Mirena, and Skyla, release a small amount of progestin similarly to a birth control pill, which usually makes periods lighter. One of them, ParaGard, also known as 'the copper T IUD,' is hormone free and lasts longer than the hormonal options, but can cause heavier periods. IUDs are more than 99% effective, but, again, do not protect against STIs.
The growing trust of IUDs is good news for women! It's important to offer many birth control options so that women may choose the method that works best for them.

 Nearly 1 in 5 teen births are
Nearly 1 in 5 teen births are  A growing number of U.S. women may be opting for intrauterine devices (IUDs) as their birth control method, a national survey finds. That's good news, researchers say, since IUDs and contraceptive implants are the most effective forms of reversible birth control.
A growing number of U.S. women may be opting for intrauterine devices (IUDs) as their birth control method, a national survey finds. That's good news, researchers say, since IUDs and contraceptive implants are the most effective forms of reversible birth control.