More intense sunlight exposure was linked with a decreased incidence of rheumatoid arthritis (RA) among women in the original Nurses' Health Study (NHS), although the more common use of sunscreen likely weakened the association in a later cohort, researchers found. Rheumatoid arthritis, or RA, is a form of inflammatory arthritis and an autoimmune disease. For reasons no one fully understands, in rheumatoid arthritis, the immune system – which is designed to protect our health by attacking foreign cells such as viruses and bacteria – instead attacks the body’s own tissues, specifically the synovium, a thin membrane that lines the joints. As a result of the attack, fluid builds up in the joints, causing pain in the joints and inflammation that’s systemic – meaning it can occur throughout the body.
More intense sunlight exposure was linked with a decreased incidence of rheumatoid arthritis (RA) among women in the original Nurses' Health Study (NHS), although the more common use of sunscreen likely weakened the association in a later cohort, researchers found. Rheumatoid arthritis, or RA, is a form of inflammatory arthritis and an autoimmune disease. For reasons no one fully understands, in rheumatoid arthritis, the immune system – which is designed to protect our health by attacking foreign cells such as viruses and bacteria – instead attacks the body’s own tissues, specifically the synovium, a thin membrane that lines the joints. As a result of the attack, fluid builds up in the joints, causing pain in the joints and inflammation that’s systemic – meaning it can occur throughout the body.
In the original Nurses' Health Study, which began in 1976, women (ages 30 to 55) living in states with the highest ultraviolet B (UVB) intensity had a 21% lower risk for RA compared with those living in states with low UVB levels according to Elizabeth Arkema, PhD, and colleagues from Harvard University.
But in NHSII, initiated in 1989 in women ages 25 to 42, no significantly lower risk was seen, the researchers reported online in Annals of the Rheumatic Diseases.
"The later birth cohort of NHSII participants (born between 1946 and 1964) were more likely aware of the dangers of sun exposure and, perhaps, had more sun-protective behavior, making residential UVB not as good a proxy for actual sun exposure in NHSII," they suggested.
Epidemiologic studies have found a correlation between an increased incidence of RA and other autoimmune diseases with higher latitude (more northern) areas of residence. In addition, experimental studies have demonstrated that UVB may suppress the immune system (which overacts in RA). Exposure to UVB also increases vitamin D synthesis in the skin, which, in turn, has altering effects on the immune system properties.
UVB flux is a measure that reflects exposure intensity based on altitude, latitude, and typical cloud cover patterns, and is expressed in Robertson-Berger units. This measure shows considerable variability in the U.S., ranging from 196 R-B units in sunny states such as Arizona and Hawaii to only 93 units in Oregon and Alaska.
Information on residence, health, diet, and lifestyle was acquired every 2 years from participants in both cohorts.
Similar findings of decreased risk for high exposure in NHS though not in NHSII were seen both for exposure levels at birth and at age 15. It thus remains unclear if the important window for UVB exposure is in childhood or adulthood. Further analyses found no significant heterogeneity according to skin type, vitamin D intake, or physical activity and body mass index.
These findings add to the increasing evidence that more intense sun exposure lowers the risk of RA, the researchers stated. "The mechanisms are not yet understood, but could be mediated by cutaneous production of vitamin D and attenuated by use of sunscreen or sun avoidant behavior," Arkema and colleagues wrote. They called for additional research to explore UVB dose intensity and timing of exposure.
EDITOR's NOTE: While the link to skin cancer and UVB exposure is well known, the increased use of sunscreen raises other health concerns that may require new approaches to find a "balance" so the benefits of a little sunshine are not totally lost.
Source reference:
Arkema E, et al "Exposure to ultraviolent-B and risk of developing rheumatoid arthritis among women in the Nurses' Health Study" Ann Rheum Dis 2013; DOI: 10.1136/annrheumdis-2012-202302.

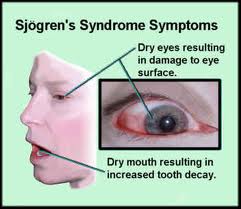 If your eyes and mouth feel as dry as a desert, there are many possible causes, such as bad air quality and certain medications. But if you have long-lasting, uncomfortable dryness in your eyes and mouth, along with fatigue or pain and swelling in some of your joints, you may have a condition called Sjögren’s syndrome.
If your eyes and mouth feel as dry as a desert, there are many possible causes, such as bad air quality and certain medications. But if you have long-lasting, uncomfortable dryness in your eyes and mouth, along with fatigue or pain and swelling in some of your joints, you may have a condition called Sjögren’s syndrome.